What is a C. diff infection?
 Last updated April 9, 2025
Last updated April 9, 2025
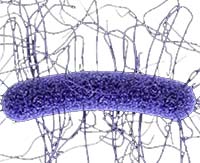
Clostridium difficile(C. difficile, or C. diff) is a specific kind of bacterial infection that causes mild to life-threatening forms of diarrhea and colitis. According to the Centers for Disease Control (CDC Link), C. diff can cause diarrhea, a fever, stomach tenderness or pain, a loss of appetite and nausea.
The bacterial infection is also called Clostridium difficile-associated disease (CDAD) or Clostridium difficile infection (CDI) to describe a number of related illnesses, such as diarrhea, colitis (irritation and swelling inside the intestine), and perforation of the colon (a hole in the intestine).
Importantly, C. diff bacteria produces toxins when the overgrow in your intestines that causes irritation to the lining of your colon, resulting in the pain, diarrhea and colitis. Toxins are what cause all the intestinal damage and pain. Many people find using toxin binders in the gut will help relieve their symptoms while their treatments are in progress.
Once you’re infected, it’s very easy to spread C. diff bacteria from one person to another, though it’s primarily spread between people by dirty hands and not washing hands before food preparation and eating. Click here for more info.
C. difficile is contagious and difficult to treat because it’s a spore forming bacteria. A spore is like a hard shell that some bacteria can wear to protect themselves in harsh environments for long periods of time (think of a seed). This hard shell makes C. difficile like a tank: it’s more difficult to treat, harder to disinfect and kill, and the spores can exist in the home for weeks or months after an infection has passed making it easy to get re-infected. Spores make C. diff hard to kill and it can’t be treated with standard antibiotics. In fact, broad-spectrum antibiotics will make the infection grow worse.
Recent C. diff facts and threats
According to the most recent CDC data in 2024, C. diff is responsible for over 500,000 infections per year in the USA. While hospital related infections are decreasing, community associated infections are increasing. C. diff causes approximately 13,000 deaths per year (these stats don’t include deaths with other contributing factors).
 Alarmingly, the death rate increased 400% between the years 2000 and 2007 due to it’s growing resistance to antibiotics.
Alarmingly, the death rate increased 400% between the years 2000 and 2007 due to it’s growing resistance to antibiotics.
80% of people catch C. difficile by visiting a hospital or other healthcare facility for treatment. Many cases of the infection are caused by the use of antibiotic drugs (such as treating a skin or sinus infection). And the majority deaths (90%) from these infections happen to those 65 years and older.
C. difficile infections can be prolonged, difficult to treat and are prone to recurring infections. C. difficile is most often a complication that appears along with other illnesses.
In September 2013, the CDC named C. diff the most urgent of all superbug infections because of it’s natural resistance to many common antibiotics and the rapidly growing number of deaths associated with this bacteria. C. difficile has continued to be named an Urgent Threat in the 2019 Antibiotic Resistant Threats report by the CDC. To read the 2019 CDC report on antibiotic resistant bacteria (the next report will come out in 2025), click here.
Q: Where does C. diff come from?
C. diff naturally lives in the environment and even in some healthy people’s intestines, without causing problems. But under the wrong conditions, like after taking broad-spectrum antibiotics, it can grow out of control and trigger serious gut infections.
C. diff has been around for decades, but it didn’t become widely known as a dangerous hospital infection until the 1970s. Since then, cases have been rising, especially in places like hospitals and nursing homes.
Antibiotics were designed to fight harmful bacteria, but overusing them can wipe out the good bacteria in your gut, giving C. diff a chance to take over. On top of that, C. diff is becoming more resistant to antibiotics, making it harder to treat. One common drug, Metronidazole (Flagyl), isn’t even recommended anymore due to declining effectiveness.
Q: Is C. difficile only found in hospitals?
Not anymore. There are actually more and more cases of C. difficile infecting otherwise healthy people who have not visited a hospital recently. According to the CDC, 20% of all C. difficile infections are community-associated; meaning they originated outside of healthcare environments.
 As you’ve probably heard, C. difficile bacteria are now in our schools, our gyms, and everywhere else that people are. Whether you’re currently infected, getting a hospital treatment or just enjoying our public places, it’s important that you be prepared with solutions that work, and have a game-plan in place on how to reduce your risk of becoming infected. More on this in a bit.
As you’ve probably heard, C. difficile bacteria are now in our schools, our gyms, and everywhere else that people are. Whether you’re currently infected, getting a hospital treatment or just enjoying our public places, it’s important that you be prepared with solutions that work, and have a game-plan in place on how to reduce your risk of becoming infected. More on this in a bit.
Q: If I get C. difficile, will antibiotics work?
Most antibiotics don’t work against C. difficile and can thus make it grow worse. There are two antibiotics (vancomycin and Fidaxomicin (Dificid)) that still work against the infection. Metronidazole has been losing it’s effectiveness. Antibiotic treatments may stop the infection, but many deal with recurrent C. difficile, relapsing into infection again after their antibiotic course is finished.
As of 2025 according to the Mayo Clinic, about 25% of people treated for C. difficile infection get sick again. The medical system will then suggest a fecal transplant if antibiotics do not work.
The Centers For Disease Control (CDC) has warned that “We are coming to the end of the antibiotic era”. Health officials clearly believe it’s just a matter of time before antibiotics can not be counted on to treat most bacterial infections. As a Microbiologist, I agree which is why I’ve spent decades looking for effective natural solutions that are hard for bacteria to be resistant to.
Fortunately, there are therapies that can be used alongside antibiotics or on their own. Natural antibiotics and probiotic therapies can work to strengthen the gut microbiome so it can “hold the line” against C. diff. These therapies can work quite well, though you may not hear about them from your doctor.
Michelle’s Recommended Probiotics
Many people with difficult infections have tried all kinds of antibiotics, special diets and probiotic supplements with no relief. Even fecal transplants can have downsides and limitations. Worse yet, many people’s doctors have run out of treatment ideas, telling their patients there’s nothing more they can do.
But you can overcome even the most stubborn infection! The answer lies in reversing how the problem was created in the first place. And you have some powerful new tools to help you succeed.
Bacillus spore-based probiotics work differently than commonly available probiotics. They survive antibiotics, they work to police your gut, targeting disease-causing bacteria while boosting the beneficial and health promoting gut bacteria like Lactobacillus, Bifidobacteria and Akkermansia species. Some Bacillus probiotics even target disease causing bacteria, including C. difficile. Michelle’s recommended probiotics are professional-strength, DNA verified and contain strains naturally found in the human gut. They don’t even require refrigeration.
C. difficile produces toxins in the gut that cause diarrhea and inflammation of the colon. Removing these toxins is a crucial, yet overlooked way to speed recovery. The Gut Restoration Pack contains Michelle’s top two C. diff. support probiotics, plus a highly targeted immunoglobulin toxin binder that’s proven to absorb C. diff. toxins A and B.
Want to Start Today?

Click the image and Save 10% on your first order and get free shipping in the U.S. on my favorite spore-based probiotics and C. diff. toxin binder. Use coupon code SAVE10. Specially formulated for C. difficile support, with five different Bacillus strains, Sac. boulardii for diarrhea support, and an immunoglobulin binder for C. diff. toxins. We provide C. diff. specific usage guides and ongoing support for our product customers. Get Michelle’s favorite Bacillus spore-based probiotics and toxin binder today.
How do I get rid of C. difficile? Why does it keep coming back?
Many people who get C. difficile have a very hard time getting rid of it. And 1 in 5 people who get infected will have multiple recurring C. difficile infections. Newer research we’ve seen also shows that Clostridium bacteria, after exposure to antibiotics, can change forms to be even more resistant to the antibiotic. This may be a big factor in it’s ability to resist antibiotic treatments.
Another reason recurring infections are so common is that most treatments do nothing to help prevent future infections. It may sound strange, but stopping your current infection is a different objective than preventing future infections. Both objectives must be addressed to stop the cycle of recurrent C. difficile infections. For more in-depth details, check out my report “10 Things You Need to Know About C. diff”, you’ll find it on the sidebar of this website.
Can I rely on natural home remedies to stop C. difficile?
C. difficile is serious business and it should be treated as such. It’s crucial to understand the big picture on how to combat these bacteria. While some home remedies work, many are not up to the task of C. difficile. And, more importantly, as I stated above, stopping C. difficile is only part of the solution.
If you have a history or C. difficile infections, it’s important that you understand how to make your body as resistant to C. difficile bacteria as possible. That’s where working with your body to naturally stop these bacteria comes in. Find out about the 3 Steps to Stop C. diff here.

About the Author – Michelle Moore, BSc
Michelle Moore is a microbiologist, holistic health educator, and author of C. difficile Treatments & Remedies. With over 10 years of experience in pharmaceutical research and over 20 years in natural medicine, she helps people overcome C. difficile and other chronic infections naturally.
References
- C. difficile Infection – Mayo Clinic
https://www.mayoclinic.org/diseases-conditions/c-difficile/symptoms-causes/syc-20351691 - About C. Diff – Centers for Disease Control Updated Dec 2024 (CDC)
https://www.cdc.gov/c-diff/about/index.html - 2019 Antibiotic Resistance Threats Report Updated April 2025 (CDC)
https://www.cdc.gov/antimicrobial-resistance/data-research/threats/index.html - C diff Diagnosis and Treatment (Mayo Clinic)
https://www.mayoclinic.org/diseases-conditions/c-difficile/diagnosis-treatment/drc-20351697 - Bacillus Coagulans GBI-30 (BC30) improves indices of Clostridium difficile-Induced colitis in mice. Fitzpatrick L, Small J, Greene W, Karpa K, Keller D. Gut Pathog. 2011; 3: 16.
- Bacillus coagulans GBI-30, 6086 limits the recurrence of Clostridium difficile-Induced colitis following vancomycin withdrawal in mice. Fitzpatrick L, Small J, Greene W, Karpa K, Farmer S, Keller D. Gut Pathog. 2012; 4: 13.
- Probiotics for Prevention of Clostridium difficile Infection. Mills J, Rao K, Young V. Curr Opin Gastroenterol. 2018 Jan; 34(1): 3–10.
- Secreted Compounds of the Probiotic Bacillus clausii Strain O/C Inhibit the Cytotoxic Effects Induced by Clostridium difficile and Bacillus cereus Toxins. Ripert G. et al. Antimicrob Agents Chemother. 2016 Jun; 60(6): 3445–3454.
Image Credits
Doctor: ©Yuri/iStockPhoto; Myths: ©CDC; 3 Steps: ©Lester Moore




 Fill in the form below to get our C. diff. tips newsletter and your free report “10 Things You Need to Know to Overcome C. difficile”.
We value your Privacy. Your email will be kept strictly confidential & secured. See our
Fill in the form below to get our C. diff. tips newsletter and your free report “10 Things You Need to Know to Overcome C. difficile”.
We value your Privacy. Your email will be kept strictly confidential & secured. See our 
